How Gut Health Affects Inflammation and Immune Health
With an increasing shift to holistic medicine and looking at the body as a whole, not a collection of individual systems, the connection between the gut and all areas of wellbeing has become more apparent. Specifically, research has begun focusing on how the diverse gut microbiome can affect inflammation and immunity in the body, and what can be done to promote good gut health.
The Impact of Gut Health
 The gut is a complex microbiome full of an estimated 100 trillion microorganisms. Many people hear of bacteria or other microorganisms in the digestive tract and worry. However, while there are some harmful microorganisms, most of them are very beneficial and necessary for good gut health.
The gut is a complex microbiome full of an estimated 100 trillion microorganisms. Many people hear of bacteria or other microorganisms in the digestive tract and worry. However, while there are some harmful microorganisms, most of them are very beneficial and necessary for good gut health.
Gut health can impact all areas of our lives, including:
- enhancing immune function
- combating obesity
- improving depressive symptoms
As you can see, a healthy gut impacts both your mental and physical health, and this knowledge helps explain why so many problems that we face can be linked back to the gut.
What Does It Mean to Have a Healthy Gut?
Having microorganisms in your digestive tract is not enough to have a healthy gut; the key is to have the correct balance of these microorganisms so that they can properly complete the tasks they need to.
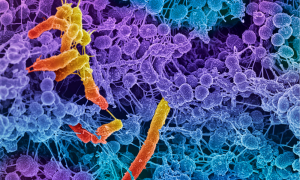 There are some bacteria that reside in the gut that are considered to be opportunistic and promote inflammation. Eating certain foods, such as animal food products, sugar, processed food, and grain-based food, has been linked with these bacteria.
There are some bacteria that reside in the gut that are considered to be opportunistic and promote inflammation. Eating certain foods, such as animal food products, sugar, processed food, and grain-based food, has been linked with these bacteria.
In comparison, the friendly bacteria in the gut produce short-chain fatty acids, which control inflammatory responses and protect the cells lining the gut.
If you have an unhealthy gut, you may relate to the following signs:
- upset stomach (gas, bloating, diarrhea, constipation, and heartburn)
- unintentional weight changes
- a high-sugar diet
- skin irritation
- sleep disturbances or constant fatigue
- food intolerances
- autoimmune conditions
With these complications in mind, let’s take a closer look at how gut health impacts the body and results in these symptoms and conditions.
Gut Health and Inflammation
Studies have found that the gut microbiome plays a role in balancing pro- and anti-inflammatory responses in the digestive system and throughout the immune system. This means that when there is an imbalance in the microorganisms of the gut, pro-inflammatory responses can increase in the body.
An increase in pro-inflammatory responses can contribute to inflammatory-mediated conditions, including:
- heart disease
- rheumatoid arthritis
- inflammatory bowel disease
- systemic lupus erythematosus
Some studies have found that diets high in animals food products, processed foods, sugar, and grain-based foods are associated with a gut microbiome that promotes excessive inflammation, showing the direct effect of what we eat on the health of our gut. In addition, the study found that a plant-based diet has the opposite effect.
Gut Health and Immune Health
Researchers have long stated that a large proportion of the immune system resides in the gut, with some even adding a quantitative estimation that 70% of the immune system is found in the GI tract.
The gut microbiome plays an important role in communicating between the gut and the immune system. When there is nothing concerning, the gut signals for the development of a healthy immune system that modulates immune responses. The immune system then populates the microbiome with health-promoting microbes.
The gut also teaches the immune system, specifically T cells, which destroy infected cells, to distinguish between the body’s own tissue and foreign entities. When the two work together, this action helps prevent an autoimmune response.
However, when the gut is unbalanced and unhealthy it does not teach the T-cells, leading to auto-immune responses. Having a weak gut lining also makes you more susceptible to new harmful invaders. So, partaking in activities that strip bacteria from the gut can impact the immune system and overall immunity.
How To Improve Gut Health
There are many lifestyle and dietary changes you can make to improve your gut health.
Get Enough Sleep
 Getting enough sleep is always one of the top tips whenever you have something wrong with your body, and for a good reason. The time the body spends sleeping is similar to performing a reset on your computer. It’s a time for the body to repair and update anything that happened during the day, putting you in the best position for the following day.
Getting enough sleep is always one of the top tips whenever you have something wrong with your body, and for a good reason. The time the body spends sleeping is similar to performing a reset on your computer. It’s a time for the body to repair and update anything that happened during the day, putting you in the best position for the following day.
If you don’t get enough quality sleep, your gut health can suffer, causing even more sleep problems. So, be sure to prioritize your sleep and focus on creating good sleep habits to get the shut-eye your gut needs.
Drink Your Water
Next to sleep, water is also important to focus on for your body’s health because of how essential it is in most functions your body does.  With the gut, in particular, studies have found that drinking enough water helps to promote a good balance of “good” bacteria in the gut while also having a beneficial effect on the mucosal lining of the intestines.
With the gut, in particular, studies have found that drinking enough water helps to promote a good balance of “good” bacteria in the gut while also having a beneficial effect on the mucosal lining of the intestines.
In short, if you want a healthy gut, make sure you’re drinking enough water.
Lower Stress Levels
 High stress levels can be detrimental to the good bacteria in your gut, so finding ways to lower stress levels can go a far way in promoting a healthy gut. Some beneficial stress-relieving activities include meditation, exercising, spending time with friends and family, aromatherapy, or spending time with a pet.
High stress levels can be detrimental to the good bacteria in your gut, so finding ways to lower stress levels can go a far way in promoting a healthy gut. Some beneficial stress-relieving activities include meditation, exercising, spending time with friends and family, aromatherapy, or spending time with a pet.
Cut Out Food Unhealthy for The Gut
As Dr. Robert H. Keller wrote in his book Glutathione – Your Best Defense Against Cellular Damage And Disease, “suffice it to say that poor nutrition results in inflammation (increased free radicals) in your intestines and has been implicated casually in every disease of aging.”
Essentially, having a diet too high in processed, high-fat, and high-sugar foods can worsen the health of your gut. If you want to improve your gut health, try removing or limiting these foods from your diet. In particular, try to focus on eating plant-based foods and lean protein.
Take A Supplement
Adding a supplement to your daily routine can help promote the health of your gut. Prebiotic and probiotic supplements provide food to the bacteria in the gut or supplement the body with additional good bacteria, respectively. Try adding a supplement to your daily schedule and see how it helps improve your gut health, your immunity, and your overall well-being. Find out the difference between probiotics and digestive enzymes.
The Gut and Overall Health
Focusing on actions that support a healthy gut will provide benefits observed across all areas of your health, both physically and mentally. If you find yourself suffering from symptoms of an unhealthy gut, take a moment to reevaluate what actions might be affecting your gut, and how you can change them so that the gut microbiome can become balanced once more.
References
Thursby, E., & Juge, N. (2017). Introduction to the human gut microbiota. Biochemical Journal, 474(11), 1823-1836. doi: 10.1042/bcj20160510
Forbes, J., Chen, C., Knox, N., Marrie, R., El-Gabalawy, H., & de Kievit, T. et al. (2018). A comparative study of the gut microbiota in immune-mediated inflammatory diseases—does a common dysbiosis exist?. Microbiome, 6(1). doi: 10.1186/s40168-018-0603-4
Bolte, L., Vich Vila, A., Imhann, F., Collij, V., Gacesa, R., & Peters, V. et al. (2021). Long-term dietary patterns are associated with pro-inflammatory and anti-inflammatory features of the gut microbiome. Gut, 70(7), 1287-1298. doi: 10.1136/gutjnl-2020-322670
Wiertsema, S., van Bergenhenegouwen, J., Garssen, J., & Knippels, L. (2021). The Interplay between the Gut Microbiome and the Immune System in the Context of Infectious Diseases throughout Life and the Role of Nutrition in Optimizing Treatment Strategies. Nutrients, 13(3), 886. doi: 10.3390/nu13030886
Yoo, J., Groer, M., Dutra, S., Sarkar, A., & McSkimming, D. (2020). Gut Microbiota and Immune System Interactions. Microorganisms, 8(10), 1587. doi: 10.3390/microorganisms8101587
Smith, R., Easson, C., Lyle, S., Kapoor, R., Donnelly, C., & Davidson, E. et al. (2019). Gut microbiome diversity is associated with sleep physiology in humans. PLOS ONE, 14(10), e0222394. doi: 10.1371/journal.pone.0222394
Vanhaecke, T., Bretin, O., Poirel, M., & Tap, J. (2021). Drinking Water Source and Intake Are Associated with Distinct Gut Microbiota Signatures in US and UK Populations. The Journal Of Nutrition, 152(1), 171-182. doi: 10.1093/jn/nxab312
Madison, A., & Kiecolt-Glaser, J. (2019). Stress, depression, diet, and the gut microbiota: human–bacteria interactions at the core of psychoneuroimmunology and nutrition. Current Opinion In Behavioral Sciences, 28, 105-110. doi: 10.1016/j.cobeha.2019.01.011




















